Why contact tracing needs to go digital
It's not just speed and coverage. It's also privacy. Unfortunately, many people think that digital means less privacy. But when it comes to privacy, nothing beats digital done right.
“People […] worry about how tech companies use the data they garner from their customers. But if covid-19 becomes a pandemic, they may well become more inclined to forgive a more nosy use of personal data if doing so helps defeat the virus.”
The Economist, February 2020
Whenever I read this quote, I realize just what a fickle thing privacy is. Those of us with the privilege of having privacy tend to take it for granted. But as the quote shows, a human right that took centuries to establish can be gone in a moment. Sure, privacy is important in normal times, the argument goes, but in the face of a severe health crisis, those concerns must unfortunately step aside.
Thankfully, digital contact tracing did not turn out to be the privacy nightmare it could have been - at least not in the places that adopted the privacy-preserving protocol built by Apple and Google (Exposure Notification). But amid concerns about digital contact tracing, what is often forgotten is that conventional contact tracing can easily become a privacy nightmare too. The problem with contact tracing in general is that it needs to collect contact data, and if that data is collected by a central actor - whether digitally or not - the potential for privacy abuse is very high.
So why bother with contact tracing in the first place? And how to make sure that it is done in a way that respects privacy? In this first post of the digital contact tracing series, I will briefly explain what contact tracing is, and why, from an epidemiological perspective, it was important to go digital. In the next post, we’ll look at the potential of digital to make contact tracing privacy-preserving, i.e. the key ideas that behind Exposure Notification. Later, we’ll look at the evidence of whether digital contact tracing worked, and what we can learn from it.
What is contact tracing?
Contact tracing is a tried and tested methodology in public health. Its ultimate goal is to stop future transmission chains, and thereby help to mitigate an outbreak, or stop it altogether. In 2003, it helped contain SARS-CoV-1. A full-blown SARS-CoV-1 pandemic would have been a public health disaster of almost unparalleled proportions, given that SARS-CoV-1 had a mortality of about an order of magnitude higher than SARS-CoV-2.
The first step of contact tracing is to identify infected individuals. This is typically done through testing, although symptomatic identification may also be a possibility. Once an infected individual - the index case - has been identified, contact tracing aims to find the individuals who have been in contact with the index case. When a contact is found, we won’t know yet whether the contact has been infected, or not. Thus, if we want to prevent future onward transmission from the contacts, then all contacts need to go into quarantine:

During the COVID-19 pandemic, contact tracing very quickly became a topic at the center of attention. As it was becoming clear that a pandemic was inevitable, contact tracing offered itself as a classical non-pharmaceutical intervention to help and slow down the spread of SARS-CoV-2. However, much of the conventional contact tracing infrastructure in public health - to the extent that it even existed - had been developed in the context of comparatively slow-moving sexually transmitted diseases (STDs) such as HIV, syphilis, and gonorrhea. In addition, no public health infrastructure was ready for the scale of contact tracing that would be necessary. For example, during the first wave of the pandemic, the Johns Hopkins Center for Health Security published an analysis suggesting that the US would need 100,000 contact tracers, which would cost about 3.6 billion dollars for one year. Similar suggestions were made in other countries. The world was simply not prepared to leverage this kind of work force for the task on such short notice.
Contact tracing nonetheless went ahead, with whatever resources were available. A key question at the time was how to define a contact. In early 2020, COVID-19 was assumed to be transmitted either through droplets, or via surfaces (we know today that the dominant transmission mode is aerosol, and that surface transmission is largely irrelevant). Based on the early 2020 assumption that droplet transmission was the dominant mode of transmission, many of the large public health bodies (WHO, US CDC, European CDC, and others) defined a contact as anyone within 1-2 meters.
It is important to keep this in mind when we evaluate the effectiveness of contact tracing. Short-range transmission is still very important, even with aerosol transmission. But aerosol transmission can also occur over longer distances. Many digital contact tracing apps did not adjust to the emerging evidence of aerosol transmission, or only very late.
Why go digital?
Even when only considering close proximity contacts, identifying such contacts is rather difficult with conventional contact tracing. For example, close proximity interactions could have easily occurred in public transport, where identifying the relevant contacts would be impossible by people’s memory alone. Furthermore, in the early days of the COVID-19 pandemic, it quickly became clear that conventional contact tracing would be too slow, given the speed at which SARS-CoV-2 spread. Correspondingly, discussions began about how the widespread use of smartphones could be leveraged to help support the fight against the emerging pandemic.
On March 12, 2020, a preprint by Ferretti et al. argued that contact tracing assisted by mobile apps could in principle, through the gain in speed, help contain the pandemic. At the time, China and a few other countries already had apps in place to help monitor and manage the pandemic. However, on a global scale, it was clear that these apps were not compatible with the privacy expectations of most countries.
Digital contact tracing thus faced a dilemma. On the one hand, speeding up contact tracing, and making it more efficient, were clearly huge potential advantages. On the other hand, privacy concerns about digital surveillance were substantial, and justifiably so. Contact tracing is already quite intrusive in the conventinal version, where individuals have to disclose who they were with, when, and where. This information, when collected centrally and electronically, would quickly offer instant access to abusive population control mechanisms to whoever holds the access keys to the data. Against this background, a number of groups started to develop protocols for digital contact tracing, assigning different importances to these issues.
The epidemiological use case
To understand the use case of digital contact tracing, let us imagine Alice as an average user of a digital contact tracing app. She goes about her daily life, and comes into contact with other people. At some point, she gets infected somewhere (not shown because it’s not important for the argument). She is not contagious yet - that will take a few days.
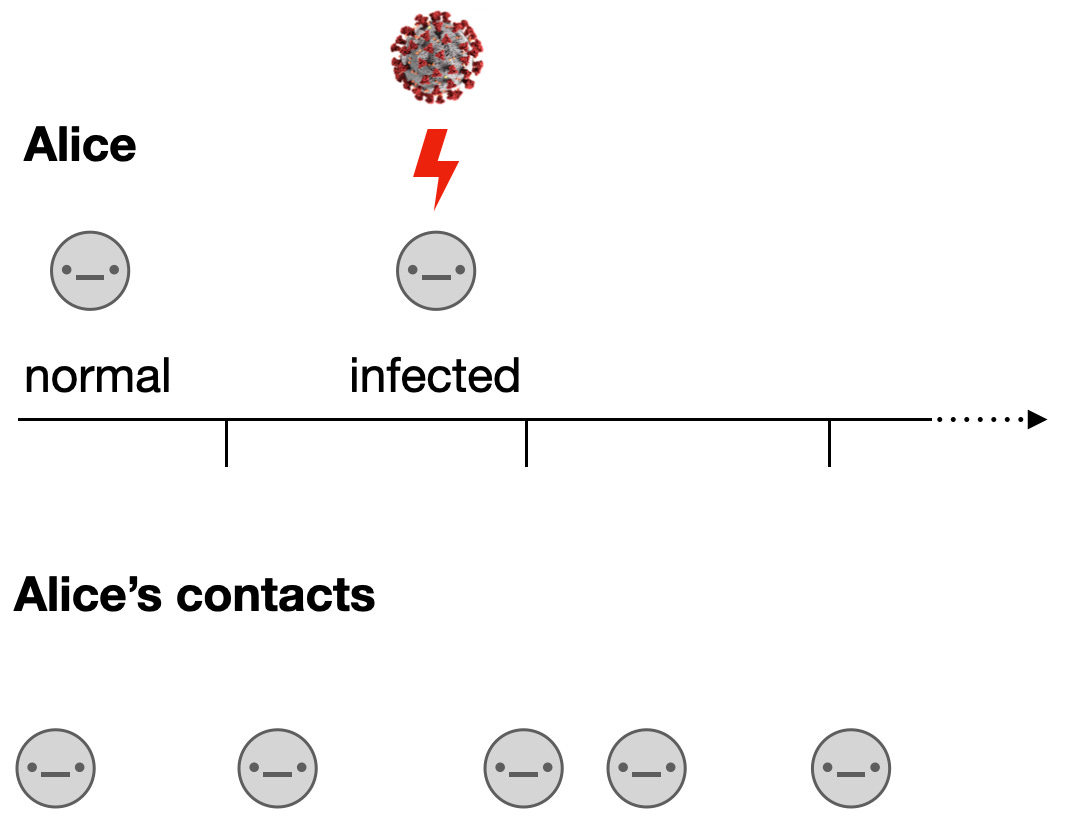
At some point, she starts to feel sick, gets tested, and receives a positive test result. At that moment, contact tracing kicks in, with Alice as the index case. Conventional contact tracing begins by a contact tracer contacting Alice, and asking her about her contacts during the previous days, up until 2-3 days before the onset of her symptoms. Alice will try to recall all the contacts she’s had in that time period. She will of course miss some, as she won’t be able to easily identify people that she doesn’t know personally. An additional challenge is that she won’t have the contact information of everyone. Once she’s given the information to the contact tracers, they will then inform the contacts about their exposure, and ask them to quarantine.
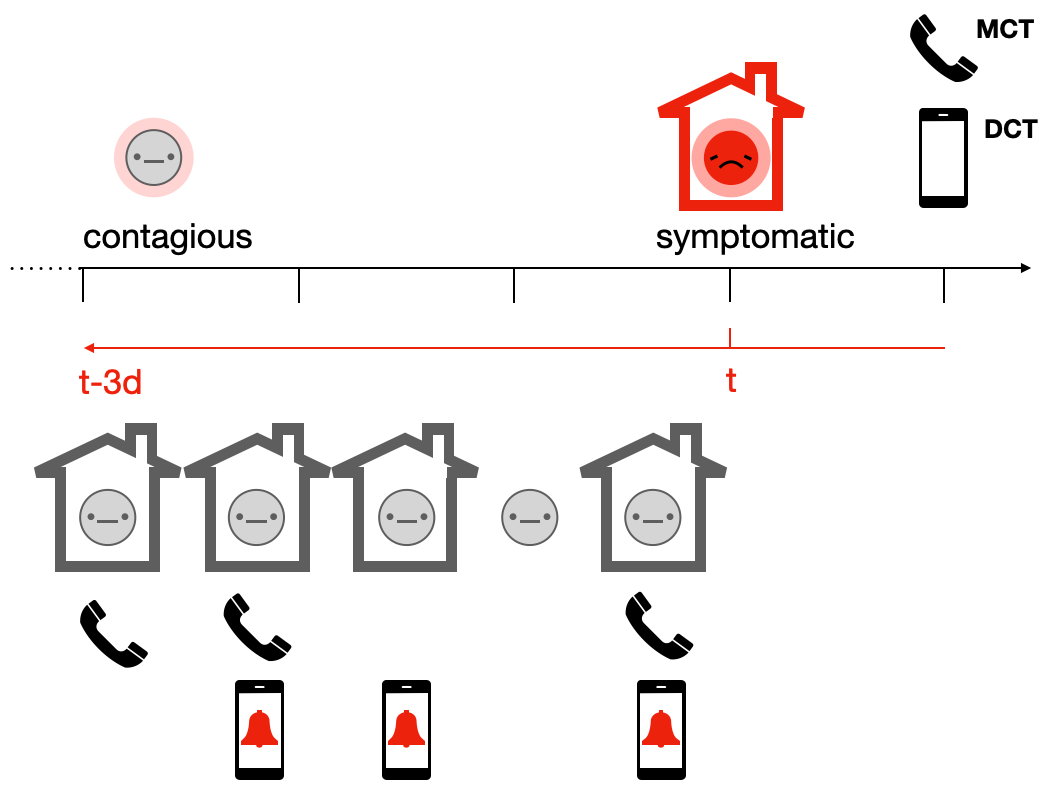
In parallel, digital contact tracing can start if Alice indicates in her contact tracing app that she has been tested positive. Her app may require a proof of her positive status - perhaps in the form of an activation code that she received with the positive test result - in order to avoid abuse of the system. Once her app knows that Alice is infected, the digital contact tracing system will notify her contacts who also used the app of their exposure, and ask them to start quarantining. Like the conventional contact tracing approach, the digital contact tracing approach will miss some contacts, either because the contacts were not properly recorded for technical reasons, or because the contact did not use a digital contact tracing app.
Ultimately, her actual contacts may fall in one of four categories: They may either be missed by both approaches; they may be contacted by either digital or traditional contact tracing; or they may be contacted twice, i.e. by both systems. Considering Alice’s example, we can see that she had five contacts during her contagious period before her isolation. Four of them are reached by the combined contact tracing efforts. If we assume that she passed on the infection to three out of the five contacts, including to the contact who was not reached by either method, the system nevertheless managed to reduce her reproduction number from 3 to 1.
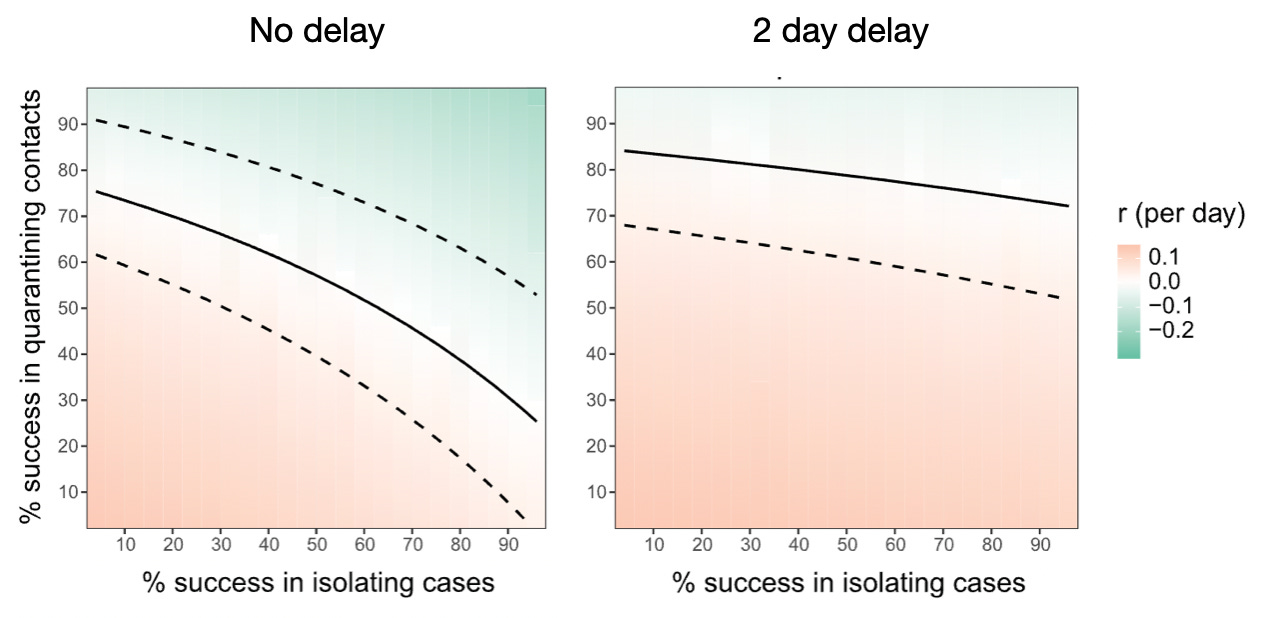
It’s quite intuitive to understand how speed matters in this system. Any delay will mean that the contacts that Alice infected might already become contagious, and pass on the infection, before contact tracing warns them of the exposure. The model developed by Ferretti et al. showed how instantaneous case isolation and contact quarantine can bring the effective reproduction number below 1, even when a substantial fraction is missed, whereas already a 2-day delay requires almost perfect success in quarantining contacts (see Figure below). Quarantining success itself depends on both index case and contact using the app; the app correctly identifying the contact; and the contact entering timely and effective quarantine. A tall order for an app, but given what was a stake, this was a path worth exploring.
While the epidemiological benefit of a digital contact tracing app was thus relatively soon established, and broadly accepted in the public health community, concerns about the privacy implications quickly became the dominant driver of most discussions. A centralized database of contacts would represent an enormous potential for abuse. In the next post of this series, we’ll look at the basics of the privacy-preserving system that ultimately made it into all iPhones and Android phones.



